What You Need To Know About Shin Splints
Are you experiencing pain around your shins or lower legs whenever you run or exercise?
Is it particularly sore after you exercise or the next day?
Is the pain stopping you from reaching your goals or performing optimally?
You might be suffering from a condition commonly known as Shin Splints.
If you want to get out of pain and get back to full function and exercise, make sure you read on to find out the 5 things you need to know about Shin Splints.
1. What Are Shin Splints?
Formally known in medical circles as medial tibial stress syndrome, shin splints are a common condition affecting runners and other exercise enthusiasts with incidence rates from 4% to 19% in athletic populations and 4% to 35% of military population (Winter’s et al, 2018). Traditionally it was thought of as an inflammatory condition, however recent studies have shown a lack of inflammation. It is now believed that shin splints are a kind of bone stress injury to the tibia or shin bone. People regularly complain of pain along the inner aspect of the shin bone aggravated by activity. Commonly an athlete will experience some relief with continued activity before pain returns after exercise and worsens the following day. Ignoring these symptoms and simply aiming to run through the pain will cause continued bone stress and potentially lead to a stress fracture!
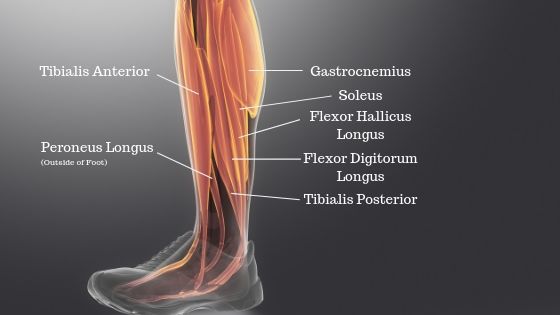
2. How and why does it happen?
Commonly, medial tibial stress syndrome is caused by repetitive stress to the periosteum of the tibia (a layer of connective tissue that surrounds the bone) beyond the body’s ability to repair it. The process is caused by spikes in training load, returning to activity early and poor biomechanics. Historically, the tibialis posterior muscle was thought to be the source of pain, but more recently the soleus and flexor digitorum longus muscles have been implicated. Activity involving excessive pronation (foot flattening out) and repetitive impact leads to chronic traction of these muscles at their insertions onto the tibia, resulting in pain. This process is accelerated when training loads exceed the capacity of the bones, muscles and tendons to resist force.
Risk Factors include;
- Training errors
- Excessive pronation
- Footwear or a change in shoes
- Altered biomechanics
- Previous injuries or stress fractures
- Exercise on hard surfaces
- Decreased flexibility

3. Early management
Currently the most effective early management is correcting training errors, managing load (how much you train), relative rest and ice. What this means is going out of your way to avoid aggravating activities and allowing the stress injury to the bone to settle down and start to recover. It is important to remember however this doesn’t mean you have to stop all exercise and “veg out on the couch”. An assessment by a trained physiotherapist can help identify aggravating activities and provide training adjustments and appropriate exercises to speed up the recovery process.

4. Why is physiotherapy so important?
In addition to playing a key role in diagnosing shin splints and leading early management, physiotherapy will focus on correcting biomechanics, improving training errors and incorrect technique. This is particularly important in the process of returning to full sport symptom free and without reinjury.
Physiotherapy plays an important role in restoring/improving strength and physio advice is critical in guiding/maintaining fitness during recovery so that you can get back to sport sooner. Your physiotherapist will also use manual therapy and sometimes taping to assist with symptom relief whilst also addressing and correcting poor muscle activation patterns impacting the way that you move, improving biomechanics and addressing weaknesses.
Our physiotherapists are experienced in the examination of the kinetic chain (the way our body moves as a whole), joint/muscle deficiencies and analysing technique to develop an individualised rehabilitation program incorporating biomechanics, strength, endurance, flexibility and injury prevention along the kinetic chain. Primarily these programs address calf/soleus/tibialis posterior strength, intrinsic foot control, core and gluteal stability, general lower limb strengthening and a progression towards functional training such as hoping, jumping and running. Integral to rehab is the safe return to sport/activity and our physios are best placed to lead a graded return to activity plan, helping reduce the risk of re-injury and subsequent issues.
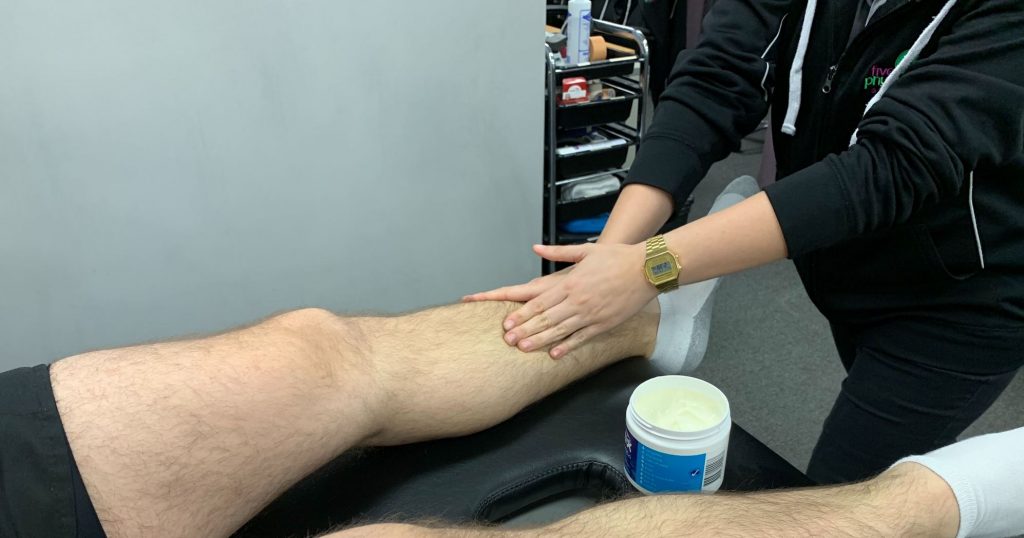
5. How easy is it to return to running and sport?
Getting back to pre-injury running and competition can be particularly difficult after lower limb overuse injuries like Shin Splints. There is a high risk of recurrence of bone stress injuries or progression towards stress fractures when athletes return to high intensity training prematurely. Injury prevention is always more effective than treatment and Yeung et al (2002) found training program alterations were the most effective in reducing the occurrence of shin splints. Brukner and Khan 2017 strongly support a graded return to running program that is based upon symptom free progression in training duration, intensity and speed. Once you have progressed through your physiotherapy program and are strong enough to start running, our physiotherapists will provide guidance in terms of how far, how often, how fast and when to increase. If we get this right, you will be competing again in no time!

Are you struggling with leg pain and need it sorted out?
GET AN ASSESSMENT & TREATMENT WITH OUR AMAZING PHYSIO TEAM.
- Get crystal clear on about what’s are the causing your pain or injury
- Understand what activities you can do without suffering consequences of further pain
- Find out the simple yet essential exercises that can help you achieve the best results
- Leave the session with the confidence of knowing exactly what to do to help you get symptom free and back to sport and activity, living life without pain & dysfunction

