Shoulder Dislocation
The shoulder is the most mobile joint in the entire body and as a result it is also the most commonly dislocated joint accounting for 50% of all major joint dislocations and it makes up the majority of traumatic sporting injuries.
Understanding the Shoulder – Anatomy
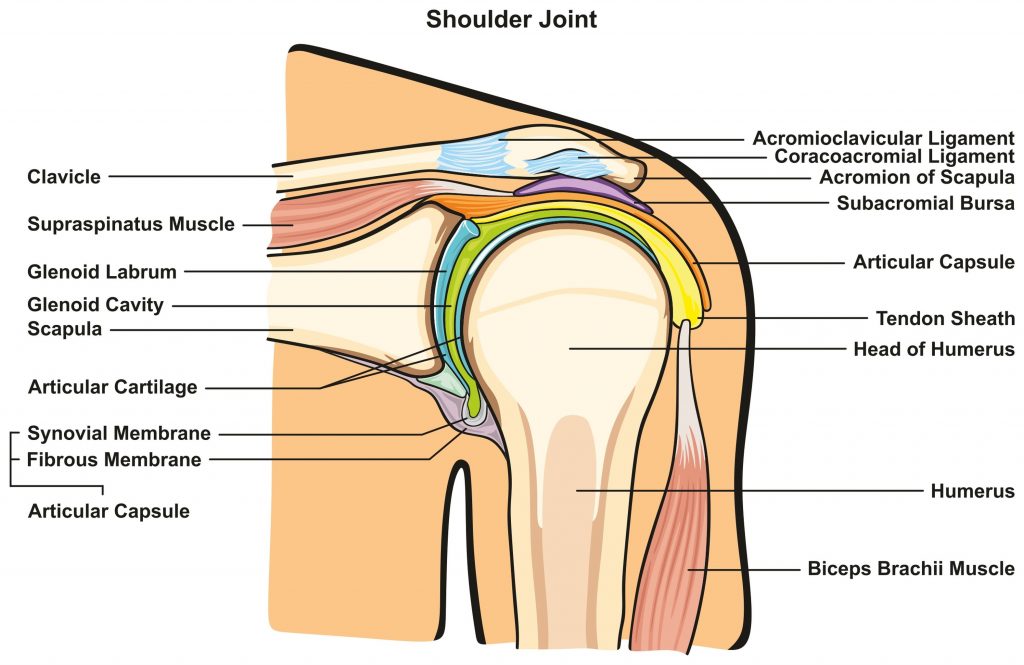
The Shoulder is a “ball and socket joint” comprised of the articulation between the scapula, humerus and clavicle. Our shoulders allow us to reach above our heads and behind our backs, lift heavy objects and move at high velocities in tasks such as throwing a ball. Due to its high degree of mobility, and in order to achieve optimal function and injury prevention, the shoulder relies on both passive and dynamic structures for stability (i.e. so it doesn’t dislocate).
The passive structures include the labrum (cartilaginous tissue), ligaments (fibrous tissue) and capsule which all function to increase the joint articulation and prevent the bones moving beyond their available range. Occasionally people will have damage or laxity to these structures creating joint instability which requires increased dynamic control.
This dynamic control is provided by the surrounding muscles, particularly the rotator cuff muscles (supraspinatus, infraspinatus, teres minor and subscapularis). These four key muscles are vital in stabilising the shoulder within its socket throughout all movements and to resist external forces that may cause a dislocation.
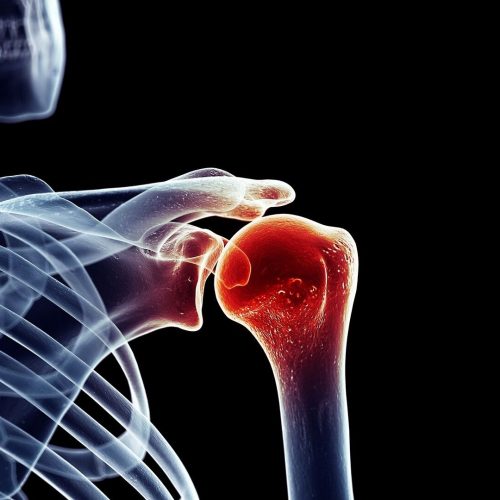
Often a shoulder dislocation is accompanied by soft tissue damage to the ligaments, rotator cuff muscles, joint capsule and labrum. In first time dislocations there can be; a Bankart lesion (82% of the time) which is damage to labrum &/or glenoid bone, or a Hills-Sachs lesion (in 71% of cases) which is an impaction fracture to head of humerus.
Is there only one type of Dislocation?
There are 3 common types of shoulder dislocation:
- Anterior dislocation — The humerus is displaced forward, toward the front of the body. It is the most common type of shoulder dislocation occurring in 95-97% of cases (Sherman, 2019). In young people, the cause is typically sports-related. In older people, it usually is caused by a fall on an outstretched arm.
- Posterior dislocation — The humerus is displaced toward the back of the body (2% to 4% of all shoulder dislocations). Posterior dislocations occur from a fall on an outstretched arm, a blow to the front of the shoulder or as a result of a seizure or electric shock.
- Inferior dislocation— The humerus is displaced downward. This type of shoulder dislocation is most rare, generally caused by various types of trauma in which the arm is pushed violently downward.
Shoulder Subluxation: It should also be mentioned that some people will “sublux” their shoulder. A Subluxation is a partial or incomplete dislocation where the humeral head slips out of its socket and back in as result of muscle weakness or a blow to the shoulder. It can occur in any of the 3 directions mentioned above, but the difference to a shoulder dislocation is the fact that the humeral head pops back into its socket. It is often due to instability.
What are the risk factors to dislocating your shoulder?
- Overhead sports such as volleyball and baseball
- Contact sports like rugby and AFL
- Previous shoulder dislocation
- Males 15 – 25 years old
- Repetitive shoulder stress activities
- Joint hypermobility and ligamentous laxity
Fall onto point of shoulder or onto outstretched arm

What to do if you suspect a shoulder dislocation?
- Seek immediate medical care to have the shoulder assessed and relocated if required (if it hasn’t popped back in itself). If it has popped back in seeing a physio is a great start, however if it is still dislocated (and believe me you’ll know it’s still out!!) presenting to the emergency department of a hospital isn’t uncommon. It is extremely important that it is relocated correctly by a professional as there are important blood vessels and nerves that can be impacted, as well as further potential damage to the bones as it relocates.
- X-rays: At a bare minimum, X-rays should be ordered to ensure no damage has occurred to the bones as well as to ensure good re-alignment and positioning after relocation.
- Further imaging such as an MRI may be required to exclude any other soft tissue pathology such as rotator cuff tear, labral tear, other muscle injury or ligament damage.
- Immobilisation: Current evidence and guidelines support shoulder reduction as soon as possible followed by sling immobilisation for a period of time determined by the doctor & physio. In a younger population Paterson et al 2010 found no benefit in sling immobilisation for periods greater than one week, whilst Shin et al 2012 supports a 2-4 week period of immobilisation for patients over 60 years old.
- Physio. After a period of immobilisation in a sling physiotherapy rehabilitation should be commenced.
What does Physio Do?
Depending on when you first present to our clinic, our physiotherapists will provide you with a thorough assessment to determine if further imaging (MRI) and specialist referral is required. Orthopaedic referral is indicated if instability is found on testing, or if a Hills Sachs or Bankart injury is found.
Initially physio helps to reduce pain and prevent compensatory movement patterns whilst beginning rehabilitation for conservative management or as preparation for those patients that require surgery. Initially this will include activating the appropriate muscles around the shoulder blade and shoulder joint to provide stability and control. This will progress to strengthening of the rotator cuff muscles and shoulder in general, improving normal muscle activation patterns and including more challenging exercises above head and with weight, progressing our patients back to their normal activities of daily living and include sport specific functional activities and return to sport guidance once appropriate.
Completing a comprehensive rehab program is essential for the safe return to sport and prevention of subsequent dislocations which are associated with surgery, arthritis and poor function (both in conservative and surgically managed patients). Other important considerations are the effects of the kinetic chain on the shoulder, and thus biomechanics and lower limb kinematics and muscle activation patterns are assessed in our clinic and strengthening programs are prescribed where indicated.
In patients that do require surgery, pre-op physio can help improve post-op outcomes by helping to improve shoulder blade stability, shoulder strength and movement.
What does the evidence say?
Unfortunately shoulder dislocations have a high rate of recurrence. Hovelius et al. 2008 in a 25-year study found that 72% of 12-22 year old’s, 56% of 23-29 year old’s and 27% of those aged 30 years+ suffered subsequent dislocations after non-operative management. Jakobsen et al. 2007 compared conservative management alone versus surgery plus rehab in first time traumatic dislocations. At 2 year follow-up, 54% of conservatively managed patients had recurrent instability compared to 3% in the surgery and rehab group. However, when deciding on management, Sachs et al. 2007 states that the strongest predictors to recurrent instability need to be considered i.e.; under 25 years of age, participation in contact sports and using arm above chest for occupation. Research shows that conservative management is progressively more successful with age whilst Rehabil et al 2017 found that a 6-week rehab program achieved full movement and comparable strength to the unaffected side highlighting the importance of physio in both conservative and surgical management.
The take home message is that if you have dislocated your shoulder and feel shoulder pain, get it relocated and then get it assessed by a physio. Physiotherapists can assess the severity of the injury from an early stage, arrange appropriate scans where necessary and help guide you arranging an orthopaedic opinion if it is required. Early physiotherapy can either prepare patients for surgery (helping to reduce compensatory movements, and improve muscle activation, strength and prognosis) or provide full rehab via conservative management but this depends on the specific case.
Do you have shoulder pain or instability that’s impacting your life?
GET AN ASSESSMENT & TREATMENT WITH OUR AMAZING TEAM OF PHYSIO’S.
- Get crystal clear about what’s causing your shoulder issue
- Understand what activities you can do without suffering consequences of shoulder pain or instability
- Find out the simple yet essential exercises that can help you achieve amazing result
- Leave the session with the confidence of knowing exactly what to do to get symptom free and back to living life to the full